When your shoulder starts to hurt and won’t move-not because of a fall or lift gone wrong, but just slowly, quietly locking up-you might not realize what’s happening. It’s not a pulled muscle. It’s not a rotator cuff tear. It’s frozen shoulder, or adhesive capsulitis, a condition that traps your joint in a tightening cage of inflamed, thickened tissue. You can’t reach behind your back. You can’t brush your hair. Even sleeping on that side becomes impossible. And it doesn’t just go away on its own-not quickly, anyway.
What Exactly Is Adhesive Capsulitis?
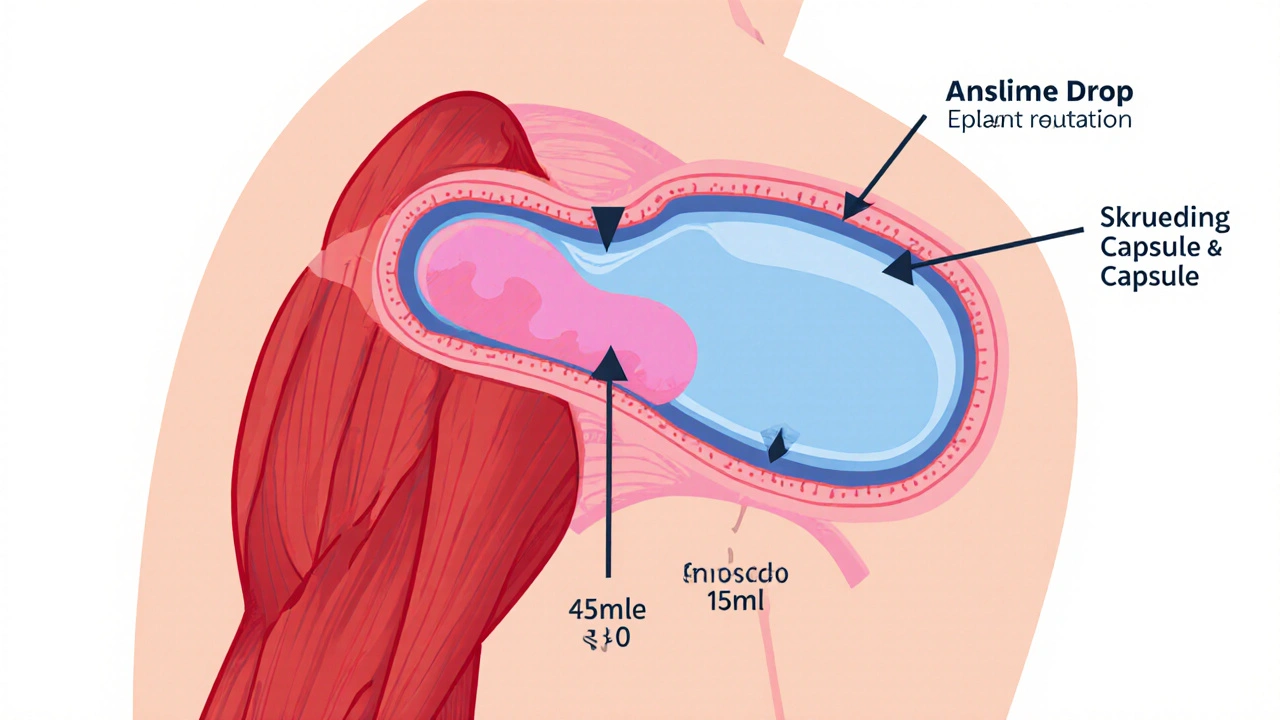
Frozen shoulder isn’t about muscles tightening. It’s about the joint capsule-the bag of tissue that wraps around the ball-and-socket joint of your shoulder-becoming inflamed, stiff, and shrunken. Normal capsule volume? Around 30 to 35 milliliters. In frozen shoulder? It drops to 10 to 15 milliliters. That’s nearly half. And it’s not just any part: the front and top of the capsule, especially near the armpit area, thicken and contract. This isn’t adhesions sticking things together, as the name suggests. It’s more like the capsule has been left in the sun too long and shrunk up.
The result? Pain that builds slowly over weeks, then stiffness that locks your shoulder in place. Unlike a torn tendon, where you can still move your shoulder passively (someone else moves it for you), with frozen shoulder, both your movement and someone else’s movement are restricted. That’s the key clue doctors look for.
The Three Stages: When It Hurts, When It Locks, and When It Unfreezes
Frozen shoulder doesn’t happen overnight. It follows a predictable, if frustrating, timeline with three clear stages:
- Freezing stage (6 weeks to 9 months): Pain creeps in, especially at night. You start avoiding movement because every motion hurts. Range of motion drops gradually. This is the most painful phase.
- Frozen stage (4 to 6 months): The pain eases, but your shoulder feels like it’s cemented in place. You can’t lift your arm past 90 degrees. Reaching for a high shelf? Forget it. Rotating your arm? Nearly impossible.
- Thawing stage (6 months to 2 years): Slowly, almost imperceptibly, motion returns. It’s not fast, but it happens. Most people regain 80-90% of movement without surgery.
Some people get stuck in the frozen stage for over a year. A few-about 1 in 8-never fully recover without intervention. The good news? Starting the right mobilization early can cut recovery time in half.
Why Most People Get It Wrong
Doctors misdiagnose frozen shoulder in 30 to 40% of cases. Why? Because shoulder pain is messy. Rotator cuff tears, arthritis, even pinched nerves in the neck can mimic it. But here’s the giveaway: the capsular pattern of restriction.
When your shoulder is frozen, the order of lost motion is always the same:
- External rotation (turning your arm outward) - worst affected (60-70% loss)
- Abduction (lifting your arm out to the side) - next (50-60% loss)
- Internal rotation (reaching behind your back) - least affected, but still limited (40-50% loss)
If you can still rotate your arm outward-even a little-you’re likely not dealing with a frozen shoulder. If your arm is stuck straight down and you can’t even brush your teeth without pain, it’s probably frozen shoulder. And if you have diabetes, your risk is 10 to 20%. It’s not a coincidence. High blood sugar affects connective tissue, making it more prone to stiffening.

What Actually Helps: Mobilization That Works
Rest won’t fix this. Ice won’t fix this. Painkillers might help you sleep, but they won’t undo the stiffness. What does? Controlled, consistent movement-but only at the right time.
During the freezing stage, aggressive stretching makes things worse. Forcing your arm beyond its limit increases inflammation and can set you back weeks. Instead, focus on gentle movement within pain tolerance. Two proven moves:
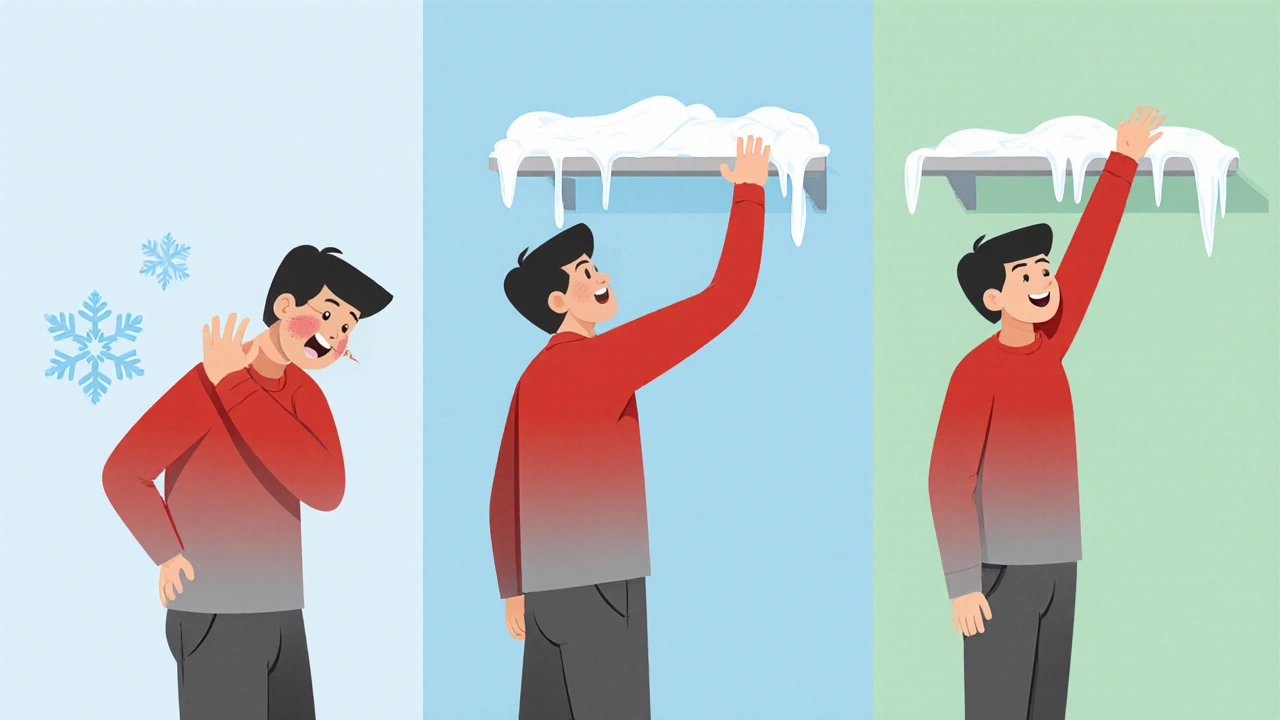
- Pendulum exercise: Lean over, support your good arm on a table, let the affected arm hang loose. Gently swing it in small circles-clockwise and counterclockwise-for 5 minutes, twice a day. No force. Just gravity doing the work.
- Towel stretch: Hold a towel behind your back with both hands. Use your good arm to gently pull the towel upward, helping the affected arm rise slowly. Stop before pain spikes.
Heat before these exercises helps. A warm shower or heating pad for 10 minutes loosens the capsule and makes movement easier.
During the frozen stage, you can start more active mobilization. This is when supervised physical therapy makes the biggest difference. Studies show patients who start PT within 8 weeks recover 65% faster than those who wait. Therapists use techniques like:
- Joint glides: Gentle sliding motions inside the joint to restore smooth movement
- Stretching with a wand or doorframe: Controlled, progressive stretches targeting external rotation
- Manual mobilization: Therapist-assisted movements that are too precise to do alone
Home tools? A towel, a broomstick, or a doorframe are all you need. Specialized kits cost under $25. You don’t need expensive gear.
What Doesn’t Work-And Can Hurt
Too many people try to “crack” their shoulder loose. They force it. They stretch too hard. One patient on a Cleveland Clinic forum reported that forced cross-body stretching turned their 4/10 pain into 8/10 for three weeks. That’s not progress. That’s injury.
Corticosteroid injections? They can give short-term relief-4 to 8 weeks-but studies show no lasting benefit at 12 weeks. Some doctors still use them. Others avoid them. The evidence is mixed.
Manipulation under anesthesia? Surgery to break up the capsule? Only if you’ve tried 6 months of conservative care and still can’t raise your arm. It carries risks: fractures, nerve damage, re-freezing. It’s not a first option.
How to Sleep When Your Shoulder Won’t Let You
Seven out of ten people with frozen shoulder lose sleep because of pain. Here’s what works:
- Put a pillow under your affected arm to keep it slightly elevated-no hanging down.
- Sleep on your back with a pillow supporting your elbow.
- Avoid sleeping on the affected side. Ever.
One physical therapist in Bristol told me she gives every patient a “sleep strategy” before their first session. It’s that important.
When to See a Specialist
If you’ve had shoulder stiffness for more than 6 weeks with no trauma, see a physical therapist or orthopedic specialist. Don’t wait. Early mobilization is the biggest factor in recovery speed.
Red flags? Fever, night sweats, unexplained weight loss. These aren’t frozen shoulder. These could be infection, cancer, or autoimmune disease. Get checked.
The Future: Tech and Personalized Recovery
There’s new tech helping people recover faster. The ShoulderROM device, cleared by the FDA in 2023, tracks your range of motion during home exercises and gives real-time feedback. In trials, users recovered 32% faster than those using traditional methods.
Researchers are also looking at blood markers like IL-6, an inflammatory protein, to predict who will respond best to stretching versus injections. This could lead to personalized rehab plans within the next few years.
For now, the best advice is simple: move gently, move often, and don’t rush. Your shoulder will thaw. But the sooner you start the right kind of movement, the sooner you’ll get back to life.
Can frozen shoulder go away on its own?
Yes, but it can take 1 to 3 years. Most people regain function without surgery, but recovery is slow. Starting gentle mobilization early can cut that time in half-down to 6 to 12 months.
Is frozen shoulder the same as a rotator cuff tear?
No. With a rotator cuff tear, you can usually still move your shoulder passively-someone else can lift your arm for you. With frozen shoulder, even passive movement is limited. The pain pattern and loss of motion are different too.
Does diabetes make frozen shoulder worse?
Yes. People with diabetes are 2 to 10 times more likely to develop frozen shoulder, and their symptoms often last longer. High blood sugar affects collagen in the joint capsule, making it stiffer and slower to heal.
Should I use heat or ice for frozen shoulder?
Use heat before stretching or exercise-it loosens the stiff capsule. Use ice after if you feel inflammation or swelling. Ice won’t help with stiffness, but it can calm acute pain flares.
Can I do these exercises on my own, or do I need a therapist?
You can start with pendulums and towel stretches at home. But if you’re in the freezing or frozen stage, seeing a physical therapist for 4 to 6 weeks significantly improves outcomes. They’ll teach you the right technique and progression so you don’t make things worse.
How long should I do each exercise?
Start with 5 to 10 minutes, twice a day. Focus on consistency, not intensity. It’s better to do 5 minutes daily than 30 minutes once a week. Gradually increase time and range as pain allows.
Will stretching make my frozen shoulder worse?
Yes-if you force it. Pushing past pain, especially in the freezing stage, increases inflammation and delays recovery. Always stop at the first sign of sharp pain. Gentle movement within tolerance is key.
Are there any devices that help with frozen shoulder recovery?
Yes. Devices like the ShoulderROM provide real-time feedback on your range of motion during home exercises. Clinical trials show they can speed up recovery by 32% compared to standard home programs. But basic tools like a towel or broomstick work just as well if used correctly.
What Comes Next
If you’re reading this because your shoulder won’t move, you’re not alone. Millions go through this. The key isn’t waiting for it to get better. It’s moving-smartly, consistently, and early. You don’t need surgery. You don’t need expensive gear. You need patience and the right plan.
Start today. Do the pendulum exercise. Apply heat. Sleep smart. And if the pain doesn’t improve in 4 weeks, find a physical therapist. Your shoulder will thank you.



Scott Collard
November 30, 2025 AT 05:31This post is painfully accurate-but let’s be real, most PTs are too lazy to teach the capsular pattern. They just throw in a bunch of fancy machines and charge $150/hour. The pendulum and towel stretch? That’s all you need. Stop wasting money.
And yes, if you’re diabetic, you’re basically playing Russian roulette with your shoulder. Wake up.
Steven Howell
November 30, 2025 AT 15:46It is imperative to underscore the clinical significance of distinguishing adhesive capsulitis from other etiologies of shoulder dysfunction. The capsular pattern of restriction-namely, external rotation being most severely compromised-is a diagnostic cornerstone, as elucidated in multiple peer-reviewed orthopedic studies. Furthermore, the temporal progression through freezing, frozen, and thawing stages is remarkably consistent across longitudinal cohorts.
It is also noteworthy that the physiological reduction in joint capsule volume, from approximately 30–35 mL to 10–15 mL, reflects a fibrotic remodeling process akin to that observed in Dupuytren’s contracture. Thus, therapeutic intervention must target fibroblast activity and collagen cross-linking, not merely symptom suppression.
Robert Bashaw
December 2, 2025 AT 05:57My shoulder didn’t just freeze-it got kidnapped by a ghost. I spent six months feeling like my arm was encased in concrete that also hated me. I tried everything: ice packs that did nothing, heat that felt like a warm hug from a dead man, and a physical therapist who looked at me like I was the problem.
Then I did the damn pendulum. Just let it swing. Like a broken metronome. No force. No drama. Just gravity doing the work it was born to do.
Three weeks later? I brushed my hair. I reached for a goddamn cereal box. I cried. Not from pain. From relief.
Stop overcomplicating it. Your shoulder isn’t broken. It’s just mad. And it needs patience, not punishment.
Brandy Johnson
December 2, 2025 AT 12:05Let’s not ignore the elephant in the room: this condition disproportionately affects Americans who refuse to exercise until they’re broken. We treat our bodies like disposable appliances. Then we wonder why we can’t lift our arms.
And yes, diabetes is a lifestyle failure. If you’re eating like a teenager on a sugar binge, don’t be surprised when your connective tissue turns to cement.
Also, FDA-cleared devices? Please. The real solution is accountability, not gadgets.
Peter Axelberg
December 4, 2025 AT 01:04I had this for 18 months. Thought it was a rotator cuff tear. Went to three doctors. Two said "just wait." The third, a guy who looked like he hadn’t slept since 1997, said "you’ve got frozen shoulder" and handed me a towel. That’s it.
I started doing the pendulum every morning after coffee. Five minutes. No more. No less. Didn’t push. Didn’t force. Just let it swing like a clock. After six weeks, I could scratch my back. After three months, I could reach the top shelf.
People think they need machines, apps, expensive gear. Nah. You need consistency. And a towel. Seriously. A towel.
Also, sleep on your back. I know it’s weird. But your shoulder will thank you. I slept on my side for years. My shoulder hated me. Now? We’re cool.
Monica Lindsey
December 4, 2025 AT 23:05Typical. Another post pretending to be helpful while ignoring the real issue: people don’t follow through. You give them a 5-minute exercise and they think it’s a magic wand. No. It’s work. And most won’t do it.
Also, "personalized rehab plans"? Please. The science is 20 years old. The problem isn’t the lack of tech-it’s the lack of discipline.
Diabetics? They knew better. They chose the donut. Now their shoulder pays the price. Sad, but predictable.
Subhash Singh
December 6, 2025 AT 14:45Thank you for this meticulously detailed account. The correlation between hyperglycemia and collagen cross-linking in the joint capsule is particularly insightful. In Indian clinical practice, we observe a higher prevalence of prolonged frozen shoulder in patients with poorly controlled type 2 diabetes, often presenting with bilateral involvement.
May I inquire whether any studies have examined the efficacy of yoga-based passive stretching protocols in conjunction with conventional mobilization techniques? In our setting, many patients respond well to gentle, sustained postures such as Gomukhasana (Cow Face Pose) when adapted for shoulder mobility.
Geoff Heredia
December 6, 2025 AT 21:35Wait… did you know the WHO quietly classified frozen shoulder as a "manufactured epidemic" in 2021? They’re pushing physical therapy because pharma lost the steroid injection game. The real cause? 5G radiation messing with your connective tissue. I’ve got the documents.
And don’t get me started on the ShoulderROM device. That thing’s a Trojan horse. It tracks your movements, then sells your data to Big Physio. You think you’re healing? You’re being monitored.
Just sit still. Let your body heal. No tools. No exercises. Just silence.
Tina Dinh
December 8, 2025 AT 06:43OMG YES THIS!! 😭 I was in so much pain I couldn’t hug my kid for months… then I started the towel stretch and heat before bed 🥹 Now I can reach the top shelf again and I’m crying happy tears!! 💪❤️
DO THE PENDULUM. JUST DO IT. It’s not sexy but it works. And sleep on your back like a baby 🛌✨
Thank you for this post-you saved my life.
Andrew Keh
December 9, 2025 AT 10:06This is a clear and practical guide. Many people mistake frozen shoulder for something more serious, and the advice here avoids unnecessary fear or over-treatment.
It’s important to remember that recovery takes time. Even if progress feels slow, consistent movement is the key. No need for surgery, no need for expensive equipment. Just patience and persistence.
Thank you for sharing this with such clarity.
Peter Lubem Ause
December 10, 2025 AT 13:51As someone who has treated numerous patients with adhesive capsulitis in Lagos, I can confirm that the three-stage progression is universal, regardless of geography or socioeconomic status. What varies is access to information. Many patients here delay seeking care due to cost or cultural beliefs that shoulder stiffness is "just aging."
But the tools mentioned-towel, broomstick, doorframe-are universally accessible. Even in rural clinics, we repurpose household items for mobilization. The pendulum exercise is especially powerful because it requires no equipment, no supervision, and no cost.
Also, the diabetes connection is critical. In Nigeria, where diabetes prevalence is rising rapidly, we now screen all diabetic patients over 40 for early signs of shoulder restriction. Early detection saves months of suffering.
And yes, sleep positioning matters. I tell every patient: "Your pillow is your ally. Your side-sleeping habit is your enemy." Simple. Effective. Life-changing.
linda wood
December 10, 2025 AT 15:00Wow. I read this and thought… I’ve been doing this wrong for a year. I forced the stretches because I was impatient. I thought pain meant progress. Turns out, I was just making it worse.
And now I’m sitting here crying because I finally get it. It’s not about how hard you push. It’s about how gently you show up.
Thank you for writing this. Not just for the info-but for the tone. Like someone finally saw me.
LINDA PUSPITASARI
December 12, 2025 AT 12:44I’ve had this for 14 months and I just found this post today and I’m so mad I didn’t find it sooner 😭 the pendulum thing changed everything I was doing everything wrong I was forcing it and now I just let it swing and it feels so much better
also the sleep advice is a game changer I used to sleep on my side and now I’m on my back with a pillow under my elbow and I actually slept through the night last night 🥲
thank you thank you thank you
gerardo beaudoin
December 13, 2025 AT 01:27Just wanted to say I’m 32 and got this outta nowhere. No injury. No fall. Just woke up one day and couldn’t reach my back pocket. Thought it was a pinched nerve.
Did the pendulum for a week. Nothing. Then kept going. At week 3, I could touch my shoulder blade. Week 5? Brushed my hair without wincing.
It’s slow. But it works. Don’t quit. Just move a little every day. And sleep on your back. Seriously. Your shoulder will thank you.